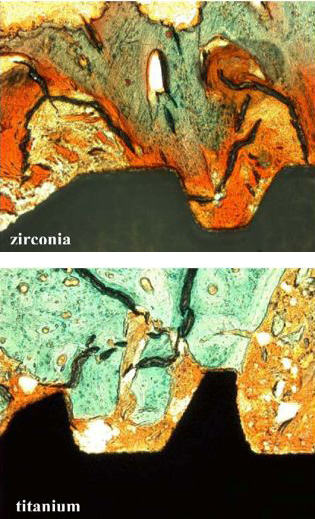
L’ostéointégration des implants céramiques
STUDIES
J Clin Periodontol. 2015 Apr;42 Suppl 16:S158-71. doi: 10.1111/jcpe.12334.
Peri-implant health and disease. A systematic review of current epidemiology.
Author information : Department of Periodontology, Institute of Odontology, The Sahlgrenska Academy at University of Gothenburg, Gothenburg, Sweden.
Abstract
BACKGROUND: To develop preventive strategies addressing peri-implant diseases, a thorough understanding of the epidemiology is required.
AIM: The aim was to systematically assess the scientific literature in order to evaluate the prevalence, extent and severity of peri-implant diseases.
MATERIAL & METHODS: Data were extracted from identified studies. Meta-analyses for prevalence of peri-implant mucositis and peri-implantitis were performed. The effect of function time and disease definition on the prevalence of peri-implantitis was evaluated by meta-regression analyses. Data on extent and severity of peri-implant diseases were estimated if not directly reported.
RESULTS: Fifteen articles describing 11 studies were included. Case definitions for mucositis and peri-implantitis varied. The prevalence of peri-implant mucositis and peri-implantitis ranged from 19 to 65% and from 1 to 47%, respectively. Meta-analyses estimated weighted mean prevalences of peri-implant mucositis and peri-implantitis of 43% (CI: 32-54%) and 22% (CI: 14-30%), respectively. The meta-regression showed a positive relationship between prevalence of peri-implantitis and function time and a negative relationship between prevalence of peri-implantitis and threshold for bone loss. Extent and severity of peri-implant diseases were rarely reported.
CONCLUSION: Future studies on the epidemiology of peri-implant diseases should consider (i) applying consistent case definitions and (ii) assessing random patient samples of adequate size and function time.
J Dent Res. 2018 Mar;97(3):259-265. doi: 10.1177/0022034517740560. Epub 2017 Nov 12.
Is Metal Particle Release Associated with Peri-implant Bone Destruction? An Emerging Concept.
Fretwurst T1,2, Nelson K2, Tarnow DP3, Wang HL1, Giannobile WV1,4.
Author information
- 1 Department of Periodontics and Oral Medicine, School of Dentistry, University of Michigan, Ann Arbor, MI, USA.
- 2 Department of Oral and Craniomaxillofacial Surgery, Center for Dental Medicine, University Medical Center Freiburg, Freiburg, Germany.
- 3 College of Dental Medicine, Columbia University, New York, NY, USA.
- 4 Department of Biomedical Engineering, College of Engineering, University of Michigan, Ann Arbor, MI, USA.
Abstract
Peri-implant diseases affecting the surrounding structures of endosseous dental implants include peri-implant mucositis and peri-implantitis. The prevalence of peri-implantitis ranges between 15% and 20% after 10 y, highlighting the major challenge in clinical practice in the rehabilitation of dental implant patients. The widespread nature of peri-implant bone loss poses difficulties in the management of biological complications affecting the long-term success of osseointegrated implant reconstructions. Metal and titanium particles have been detected in peri-implant supporting tissues. However, it remains unclear what mechanisms could be responsible for the elicitation of particle and ion release and whether these released implant-associated materials have a local and/or systemic impact on the peri-implant soft and hard tissues. Metal particle release as a potential etiologic factor has been intensively studied in the field of orthopedics and is known to provoke aseptic loosening around arthroplasties and is associated with implant failures. In dental medicine, emerging information about metal/titanium particle release suggests that the potential impact of biomaterials at the abutment or bone interfaces may have an influence on the pathogenesis of peri-implant bone loss. This mini-review highlights current evidence of metal particle release around dental implants and future.